|
|
|
 |
|
| Welcome | Contact | Getting Started | Site Map | Project | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 |
Topic 6 - Biological Effects and Risk
Biological Effects |
- Hall, Radiobiology for the Radiologist
- Cember, Ch. 7
Radiobiology
- The study of the action of ionizing radiations on living things.
- Biology primer see http://www.biology.arizona.edu/cell_bio/tutorials/cell_cycle/main.html
- Absorption of energy in biological material leads to excitation
or ionization.
- excitation: raises electron to higher energy state without ejecting it from the atom. Radiations can be emitted from this process
- ionization: ejects electron from the atom. Radiation is also released in the process
Energy absorption in Radiobiology
- Photons absorbed
- Energy deposited in cells and tissues
- unevenly in discrete packets
- typical energy per ionizing event ~ 33 eV
- Typical C=C bond is 4.9 eV
- Where does remainder go?
Energy Absorption
- Consider 70 kg person
- LD50/60 = 4 Gy (400 rad)
- Energy absorbed: 70 kg · 4 J kg-1 = 280 J
- What is the caloric equivalent of 280 J?
- Calorie, metric unit of heat measurement. The small, or gram, calorie (cal) is the amount of heat required to raise the temperature of 1 g of water from 14.5° to 15.5° C.
- 1 cal equals 4.1840 joules (J)
- 280 J / 4.186 = 67 calories
- What would be the temperature rise in the body from this energy deposition?
- Why is this a lethal dose?
Direct and Indirect Action
- Biological effects of radiation result principally from damage to
DNA
- DNA the critical target
- Target can be directly damaged by radiation
- Target can be indirectly damaged
Direct and Indirect Action of Radiation in Biological Systems
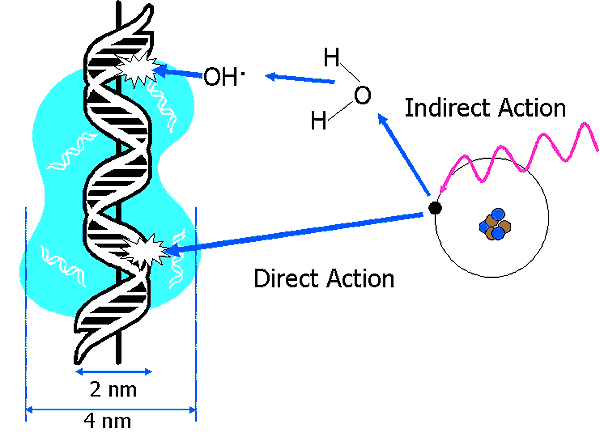
Indirect Action in Detail
- H2O -> H2O+ + e-
- H2O+ is an ion (electrically charged)
- H2O+ is also a free radical
- unpaired electron in outer shell
- very reactive
- H2O + H2O +-> H3O+ + OH·
- OH· (hydroxyl radical)
- 9 electrons, very reactive
- free radical
Chain of events in X-ray absorption
Incident X-ray beam
ß
Fast electron (e-)
ß
Ion Radical
ß
Free Radical
ß
Chemical changes from bond breakage
ß
Biological Effects
Time Scale of Events
- Initial ionization: 10-15s
- Ion radical lifetime: 10-10s
- Free radical lifetime: 10-5s
- Breakage of bonds and expression of biological effects: hours, days,
months, years
- cell killing: hours to days
- oncogenic: years
- mutation in germ cell: generations
Contrast Between Neutrons & Photons
- X and g-rays
- indirectly ionizing
- produce fast moving secondary electrons
- Neutrons
- indirectly ionizing
- produce recoil protons, alphas, and heavier atoms
Neutron Interactions
- Direct action dominates for densely ionizing radiations
- 20 charged particles result in a dense column of ionizations more likely to interact with the DNA
- Free radicals are also produced
- Recoil protons, alphas, heavy fragments
- massive -similar size to medium
- densely ionizing
- positively charged
Direct and Indirect Action of Radiation in Biological Systems - Neutrons
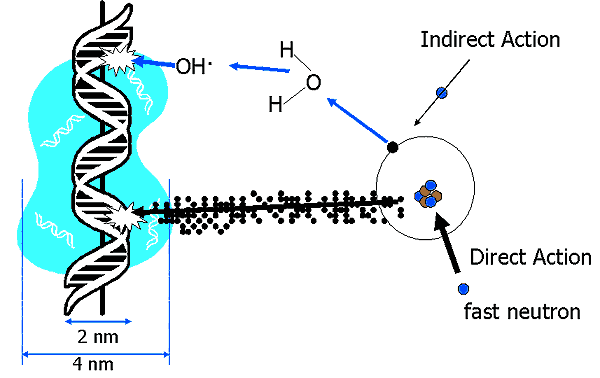
Summary of Pertinent Conclusions
- X- and g-rays
- indirectly ionizing
- produce fast recoil electrons
- Neutrons are indirectly ionizing
- produce fast recoil protons, a-particles, hcp
- Biological effects due to
- direct action
- indirect action
- about 2/3 of X-ray damage is by indirect action
- Photons - Indirect action dominates
- Heavy particles - direct action dominates
Radiobiological Studies
- Methods Used to Assess Radiation Effects
Radiation Effects: Determining the Mechanism of Cell Killing
- Sensitive sites are
- The nucleus
- Not the cytoplasm
- Early studies
- microbeams
- nonmammalian cells
- cytoplasm or nucleus irradiated
Nucleus vs Cytoplasm - Radiosensitivity
- Habrobracon (wasp) eggs

- Average # of incident as
needed to reduce hatchability to 37%:
- nucleus: 1
- cytoplasm: 17.6 x 106
Irradiation of Cytoplasm
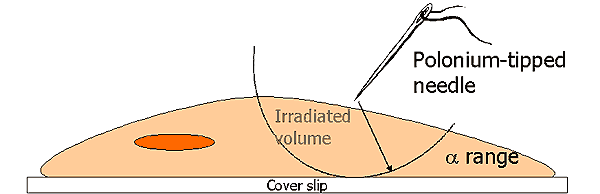
- Irradiation of part of cytoplasm of a cultured Chinese Hamster cell by a-particles from a polonium-tipped micro-needle
- The irradiated volume is limited by the range of the particles
Other Evidence for Chromosomes As Primary Target in Cell Killing
- Cells killed by radioactive tritiated thymidine incorporated into DNA
- Structural analogues of thymidine when incorporated substantially increase radiosensitivity of cells
- Transplantation of irradiated nucleus into unirradiated cell is lethal at doses that an unirradiated nucleus can survive
Other Methods in Radiation Effects Research
- Methods for assessing dose response
- in vitro:
- cell survival curves
- irradiate seeded cells
- assess colony formation
- determine surviving fraction
- cell survival curves
- in situ -
- clonogenic endpoints
- clones regrowing on irradiated skin
- Whole animal studies
- clonogenic endpoints
- in vitro:
In Situ Tests - Clonogenic Endpoints
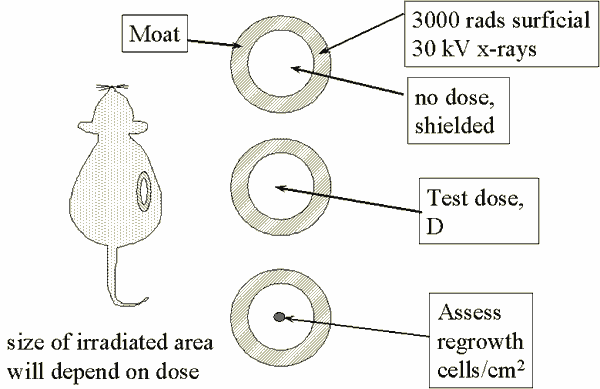
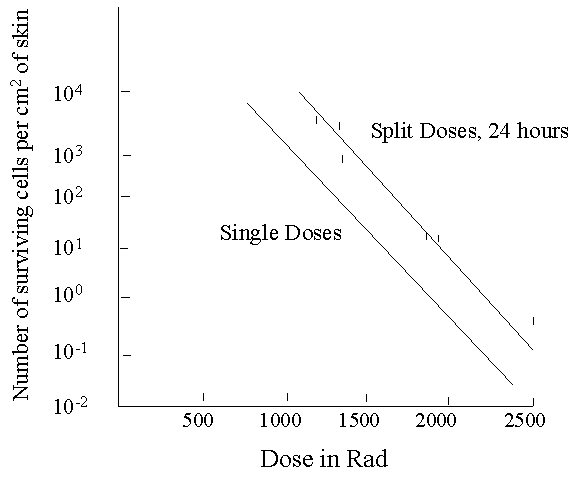
Skin Studies - Example Data
Another functional endpoint
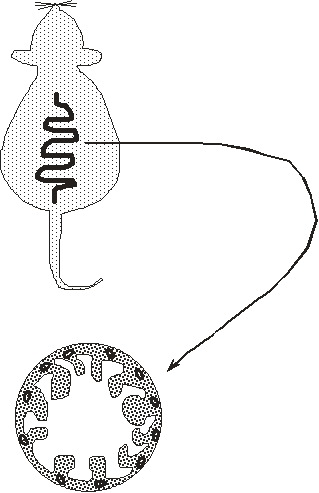
- Expose animals to graded dose
- Wait 3 days
- Sacrifice animal
- Thin-section jejunum
- Score for regenerating crypts per circumference
Fractionating dose extends survival
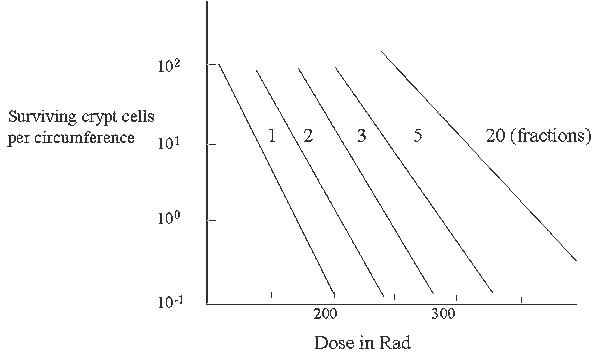
What Have We Learned in Radiation Response of Tissues
- Response is a function of
- Cell sensitivity
- Cell population kinetics
- Cell survival curves irrelevant in highly differentiated cells (no mitotic future)
- Closed population of mature cells very resistant
- Self-renewing tissues: dividing cells are weak link
Cell Sensitivity - Cell Type Matters
Cell Types
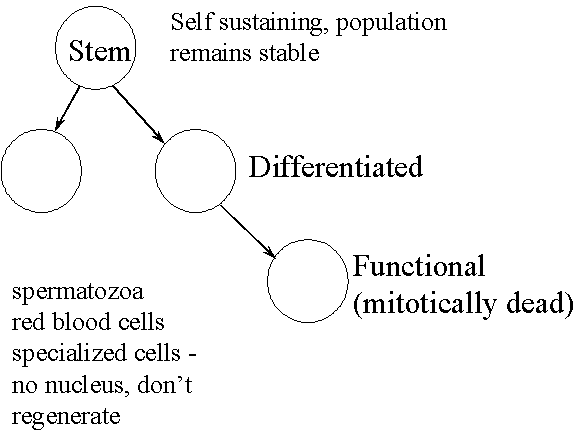
Tissue response, contd
- Loss of reproductive capacity occurs after a few Gy
- Impact to tissue/organ after dosing depends on how well it can function with reduced number of cells
- Time between dose & expression of damage is variable
- lifetime of mature cell
- time for stem cell to mature to functional state
Radiation Response, contd
- Blood cells
- lifetime 3-4 months
- damage to stem cells not evident until red blood cell pool dies off
- Intestinal epithelium
- mature villi - short lifespan
- impact obvious within few days
Parenchymal Cells & Connective Tissue
- Parenchymal cells
- perform unique function of particular tissue
- supported & held in place by connective tissue
- supplied with O2 & nutrients by blood vessels
- Casarets classification
- connective tissue, blood vessels intermediate in sensitivity between most sensitive and most resistant parenchymal cells.
- Radiation effects parenchyma, connective tissues, vasculature, controversy on which responsible for late effects
Casarets Classification of Mammalian Parenchymal Cell Sensitivity
- Type
- I - VIM
- II- DIM
- III RPM
- IV FPM
- Example
- crypt
- myelocytes
- liver
- nerve
- Sensitivity
- High
- Intermediate
- Moderate
- Low
Supporting structures (connective tissues, endothelial cells)
Noted exception to the classification - small lymphocyte, which disappears
after small doses. It doesn’t divide, yet is one of the most sensitive
mammalian cells.
Cell Sensitivity - Population Kinetics
The Cell Cycle
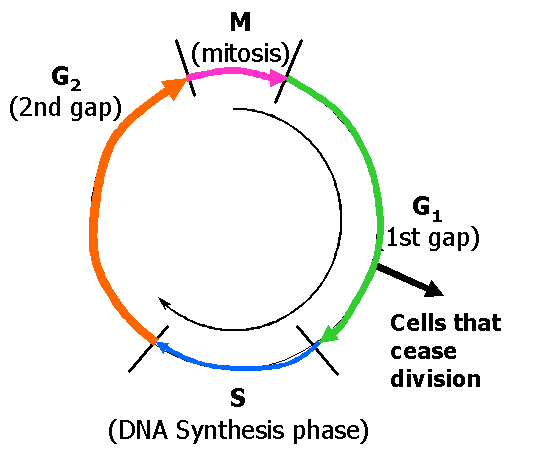
- An ordered set of events, culminating in cell growth and division into two daughter cells
- Tc, full mitotic cycle
- Only mitosis can be distinguished when examining cells under a scope
-
- chromosomes are condensed
- mitosis ~ 1 hour
- Radiography used to study
Mitosis
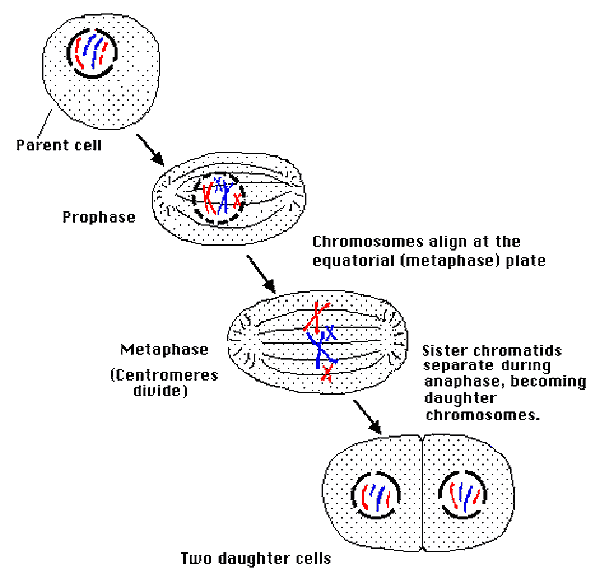
Cell Cycle Times
- Radiography, other techniques
- used to view cells
- help identify cell cycle length
- All proliferating mammal cells have
- mitotic cycle
- followed by G1
- period of DNA synthesis (S)
- G2
- mitosis repeats
Length of Cell Cycle
- M, S, G2 vary little between cells
- Tc varies 10 hours - 100s of hours - mainly due to G1
| Phases of the Cell Cycle for two Commonly used Cell Lines in Vitro (hours) | ||
|---|---|---|
| Hamster Cells | HeLa Cells | |
| TC | 11 | 24 |
| TM | 1 | 1 |
| TS* | 6 | 8 |
| T02 | 3 | 4 |
| T01 | 1 | 11 |
*In all cell lines cultured or in vivo, S never exceeds 15 h
X-Ray Sensitivity of Synchronous Cells
- Chinese Hamster cells in culture
- Irradiated with 6.6 Gy after mitosis
- time of exposure varied
- cells irradiated at different stages in cell cycle
- Shown in next figure
- Key points
- mid-late S least sensitive
- Irradiated with 6.6 Gy after mitosis
X-Rays & Synchronously Dividing Cell Cultures after 6.6 Gy
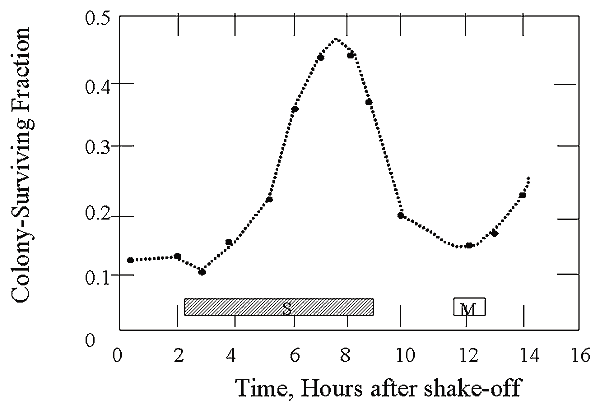
Fraction of HeLa cells surviving a dose of 3 Gy
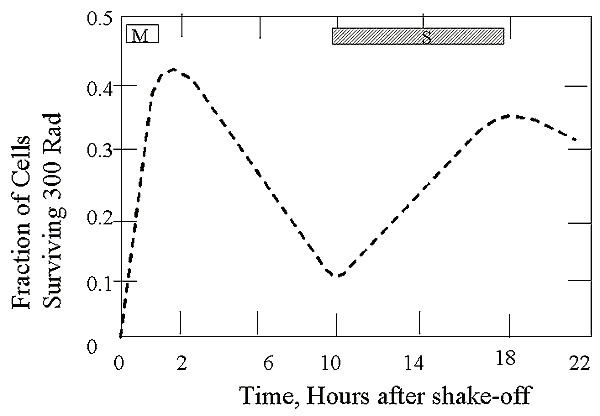
Key Differences between HeLa & Chinese Hamster Cells
- Cycle time
- Tm
- Ts
- Tc
- TG2
- TG1
- Hamster
- 1
- 6
- 11
- 3
- 1
- HeLa
- 1
- 8
- 24
- 4
- 11
- For S phase, HeLa & Hampster are similar
- Major Difference is Length of G1
Radiosensitivity & Mitotic Cycle
- Sensitivity
- Cells most sensitive close to mitosis
- Resistance greatest in latter part of S
- For long G1s, there is an early resistance period followed by sensitive one at the end of G1
- G2 ~ M in sensitivity
- Probably Repair is the key
Whys & Wherefores of Sensitivity
- Cellular progression controlled by checkpoint genes
- ensure completion of events prior to progression through cell cycle,
- at G2 cells are halted to inventory & repair damage before mitosis
- cells where checkpoint gene inactivated
- these cells move directly to mitosis with damaged chromosomes
- are more sensitive to UV or g radiation or any DNA damaging agent
Cell Cycle Summary
- Cell cycle components
- M, G1, S, G2
- Cycles in culture
- crypt cells, 9 - 10 hours
- stem cells (mouse skin) 200 hr
- due to G1
- Cells most radiosensitive in M, G2
- Resistant in late S
Implications of Cell Cycle Sensitivity & Tumor Therapy
- Tumor cells initially asynchronous
- (distributed throughout cycle)
- Deliver dose
- Kill sensitive cells (M)
- Radiation ~synchronizes population
- Allow cells to progress
- Sensitized cycling population
- Time next dose to sensitive phase
- Good in theory
- Need tumour kinetics to accomplish
Age-Response Implications, contd
- Time next dose to correspond to sensitive phase of tumor - maximize cell killing
- Sensitization due to reassortment
- Therapeutic gain (tumors are rapidly dividing as opposed to most normal tissues)
Effect of Oxygen on Cells
- OER
- oxygen enhancement ratio
- aerated cells more sensitive
- typical values 2.5 - 3 for g and x-rays
- oxygen reacts with free radicals to produce peroxide - non repairable damage
- G1: 2.3 - 2.4
- S: 2.8 - 2.9
- G2 intermediate
- Implications are in radiation therapy
Oxygen Fixation Hypothesis
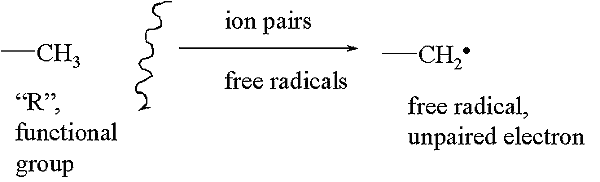
In general, the free radical reactions go like this:
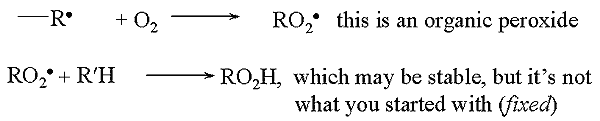
O2 Concentration & X ray Impacts
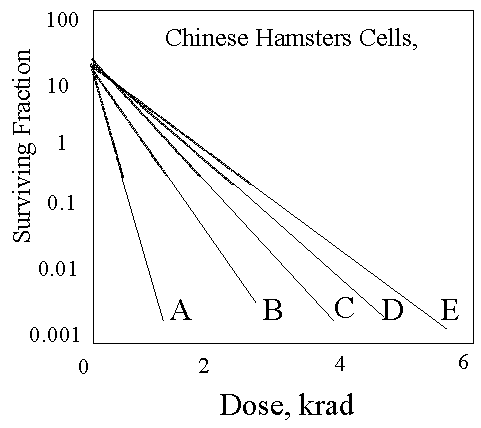
- Bacteria & mammalian systems show similar effects
- A: air (210,000 ppm)
- B: 2200 ppm O2(0.25%)
- C: 355 ppm O2
- D: 100 ppm O2
- E: 10 ppm O2
Radiosensitivity & O2 Concentration
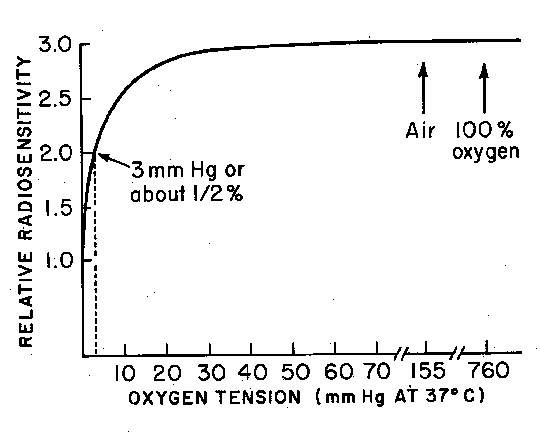
- O2 levels
- 20 % normal
- 16% dizziness
- 10% immediate unconsciousness
- 2% is ~ plateau
- 0.5% is 50% effect
- Doesnt take much for impact
Oxygen Movement Through Tissues
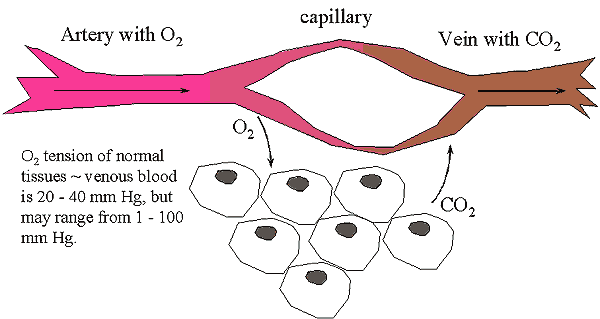
- Oxygen passes from blood to capillaries to tissue cells.
- CO2 passes from tissue cells to capillaries to blood
- Hemoglobin binds with O2 in O2 rich environment (lung)
- Gases diffuse from high to low concentration
- O2 diffuses from blood to tissue fluid
- Same, in reverse for CO2
Diffusion of Oxygen Through a Capillary
Oxygen Movement, contd
- O2 is on plasma & hemoglobin
- small fraction on plasma
- immediately available to diffuse to cells
- remainder is with hemoglobin
- Many cells are borderline hypoxic
- Liver
- Skeletal cells
Conditions of Hypoxia
- Chronic hypoxia
- Limited diffusion distance of O2 through respiring tissues
- Cells may be hypoxic for a long time
- Tumors may outgrow blood supply, have O2 starved regions
- Acute
- Blood vessels can be temporarily shut down
- Rapidly reopen to resupply tissues
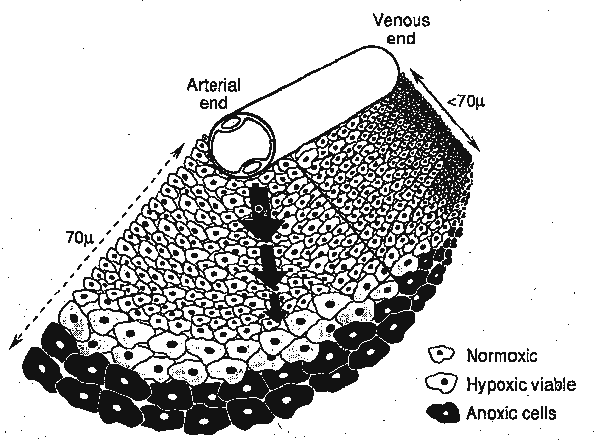
Significance of O2 Effect and Solid Tumors
- Solid tumor growth limited by oxygen supply
- Often with necrotic (dead) center
- As tumor grows, necrotic center expands
- Thickness of healthy sheath remains constant
- Estimated diffusion distance of O2 in respiring tissue is 70mm
Thomlinson & Gray (1955) Key Paper

Reoxygenation in Tumors
- Mouse Sarcoma
- Initial survey 14% of tumor cells hypoxic
- Series of dose fractions 5 dose, 1.9 Gy/day
- Reassessed fraction hypoxic cells (18%)
- Similar experiment,
- M-Th, 4 dose fractions,
- Next day hypoxic cells 14%
- Implies fraction of hypoxic cells before/after therapy are same
Reoxygenation
- What is going on?
- Treatment kills oxygenated tumor cells
- Hypoxic ones become oxygenated
- This is a good thing
- Hypoxic cells reoxygenate after radiation therapy and become radiation sensitive
Process of Reoxygenation
- If reoxygenation occurs, then the presence of hypoxic cells wont significantly impact the outcome of the multi-fraction regime
Mechanism of Reoxygenation
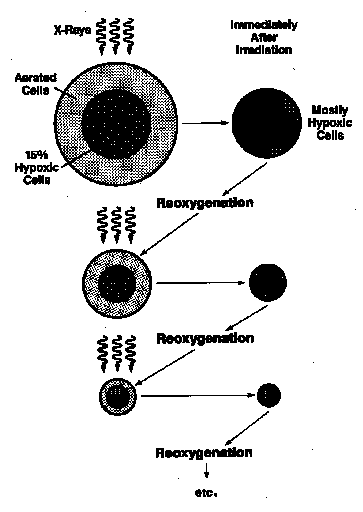
- Reoxygenation variable
- Fast (hours)
- Slow (days)
- Some tumors exhibit two component process
- related to type of hypoxia being reversed
- chronic
- acute
- Slow, long term
- Revascularization occurs (dead cells are broken down and removed)
- Tumor shrinks so all within O2 diffusion zone
- Applies to chronically hypoxic cells
- Fast, short term
- Reoxygenation of acutely hypoxic cells
- Blood supply reopens & rapid reoxygenation occurs
Significance for Radiotherapy
- Tumors (animal) include
- Aerated
- Hypoxic cells
- Hypoxia confers protection from
- X-rays
- Chemotherapeutic agents (e.g., bleomycin)
- Presence of O2 enhances cell killing
- Reoxygenation of hypoxic cells could enhance cancer treatment through radiation therapy
- Reoxygenation pattern not well known for many systems
- If human tumors reoxygenate quickly
- Multifraction therapy could deal with resistant subpopulation
- Dosing at later intervals would maximize killing
- Human tumor data not available
- Reoxygenation suggested from multifraction therapies
- 60 Gy in 30 treatments eradicates many tumors where cure not expected
Other Factors Affecting Dose Response
- Relative Biological Effectiveness
- General rule - high LET radiation more damaging than low LET
- Different radiations can be compared:
- RBE = Dx/D
- D is dose of a given radiation required to produce a specific biological endpoint
- Dxis the X-ray dose needed under same conditions to produce same endpoint
- RBE results used to produce Q, wR values
- Dose Rate
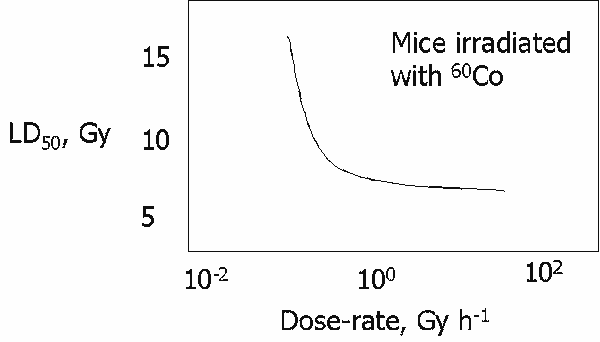
Other Factors Affecting Dose Response
- Chemical Modifiers
- Sensitizers
- Oxygen
- Radioprotectors
- Sulfhydryl compounds (free radical scavengers)
- Sensitizers
- Heat
Radiation Effects on Living Systems
- Varies with:
- dose magnitude
- duration of exposure
- region exposed
- Responses categorized:
- stochastic: mutagenic/carcinogenic/ teratogenic
- nonstochastic (deterministic) - threshold
Radiation Effects
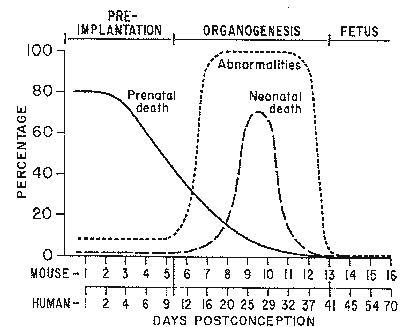
- Cellular Level
- cell function
- cell division
- chromosomal damage
- neoplastic transformation
- Organs
- prompt (death)
- delayed (fibrosis)
- Individual
Factors Affecting Cellular Radiosensitivity
- Cells that divide more rapidly are more sensitive to the effects of radiation ...
- essentially because the resulting effect is seen more rapidly.
Factors Influencing Biological Effect
- Total absorbed energy (dose)
- Dose rate
- Acute (seconds, minutes)
- Chronic (days, years)
- Type of radiation
- Source of radiation
- External
- Internal
- Age at exposure
Factors Influencing Biological Effect
- Time since exposure
- Area or location being irradiated
- Localized (cells, organ)
- Extremities (hands, forearms, feet, lower legs)
- Entire body (trunk including head)
- Superficial dose (skin only - shallow)
- Deep tissue (deep dose)
Categorizing Exposure
- Acute
- Single, large, short-term whole-body dose
- Characterized by four sequential stages
- Initial (prodromal) - lasts 48 hrs
- Latent - 48 hr to 3 weeks
- Manifest illness - 6 to 8 weeks postexposure
- Recovery (if death does not occur) weeks-months
- Chronic
- Lower, protracted dose
Terms
- Acute exposure
- dose received in a short time (seconds, minutes)
- Acute effects
- symptoms occur shortly after exposure
- Chronic exposure
- dose received over longer time periods (hrs, days)
- Delayed effects
- symptoms occur after a latent (dormant) period
- Somatic effects
- those which occur in the person exposed
- Genetic effects
- those which occur in the offspring of exposed persons
- Stochastic effects
- likelihood of effect is random, but increases with increasing dose
- Non-stochastic effects
- likelihood of effect is based solely on dose exceeding some threshold
Symptoms of Acute Radiation Sickness
- Three categories (E. Hall, 1994)
- Hemopoietic: 3-8 Gy LD50/60
- radiation damages precursors to red/white blood cells & platelets
- prodromal may occur immediately
- symptoms: septicemia,
- survival mixed
- examples include Chernobyl personnel (203 exhibited symptoms, 13 died)
- Gastrointestinal : >10 Gy
- radiation depopulates GI epithelium (crypt cells)
- abdominal pain/fever, diarrhea, dehydration
- death 3 to 10 days (no record of human survivors above 10 Gy)
- examples include Chernobyl firefighters
- Cerebrovascular : > 100 Gy
- death in minutes to hours
- examples include criticality accidents
- Hemopoietic: 3-8 Gy LD50/60
Delayed Effects
- Some biological effects, either from acute or chronic exposure may take a long time to develop & become evident in exposed individual.
- Called delayed or late, somatic effects
- Cancer
- Leukemia
- Bone Cancer
- Lung Cancer
- Life Shortening
- Cataracts
Other Effects
- Mental Retardation
- Genetic Effects
Sources of Human Data
- Considerable body of data exists
- Atomic-bomb survivors
- RERF
- 93,000 survivors
- 27,000 nonexposed comparators
- Atomic-bomb survivors
- Medical patients
- Therapeutic
- Thymus treatments - increase in thyroid tumors
- Tinea capitis (ringworm of the scalp)- 10,000 children- 6 fold increase in malignant tumors of thyroid
- Ankylosing spondylitis (inflammatory arthritis that affects the spinal joints) - 14,000 patients - increase in leukemia
- Diagnostic
- Therapeutic
- Body of data, contd
- Radium dial painters - several hundred, bone cancer
- Uranium miners - thousands - lung cancer
- Accidents
- Critical assemblies
- Particle accelerators
- Radiation devices
- Weapons fallout
- Chornobyl
Examples of Dose-Response Relationships
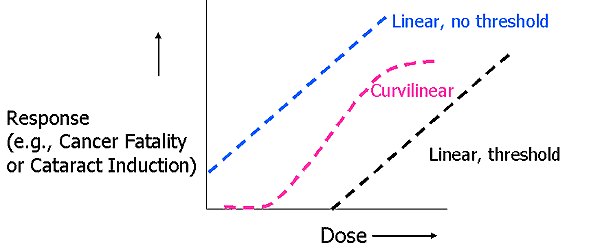
Non-Stochastic (Deterministic) Effects
- Occurs above threshold dose
- Severity increases with dose
- Alopecia (hair loss)
- Cataracts
- Erythema (skin reddening)
- Radiation Sickness
- Temporary Sterility
Stochastic (Probabilistic) Effects
- Occurs by chance
- Probability increases with dose
Dose Response: Radiation Carcinogenesis
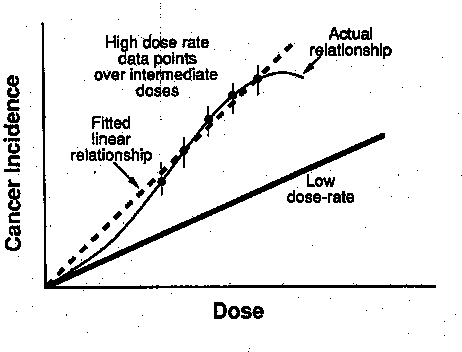
- Two effects of radiation exposure:
- deterministic (threshold)
- stochastic: cancer
- Radiation Standards
- set below threshold
- set to limit stochastic risk
- Controversy on Risk
- possibility of threshold
- low-dose data limited
Linear non-threshold hypothesis
- Fits data
- Single hit effect
- Accepted by most regulatory bodies
- Conservative
- Basis of current regulations
Biological Effects Summary:
- What We Know and What We Dont Know About Radiation Health Effects
- Borrowed from a talk by G. Roessler An Educational Briefing By The HEALTH PHYSICS SOCIETY Specialists In Radiation Safety March 28, 2001
Health Effects of Ionizing Radiation
- More known about radiation effects than effects from any other potentially toxic substance -- more than chemicals
Sources of Information
- Molecules and Cells
- Animals
- Humans (Epidemiological Studies)
- Medical
- Occupational
- Hiroshima and Nagasaki
Time Frame of Effects
- Physical -- less than seconds
- Chemical -- seconds
- Biological -- seconds to many years
- Reactions with molecules, cells
- Tissue changes
- Cancer, leukemia
Effects
- The radiation may enter the body but miss important targets
- The radiation may not cause any damage to a target
- The damage may be repaired
- A damaged cell may die
- A damaged cell may be changed (mutated)
- High Doses
- May Lead to Early Effects or Death
- Low Doses
- Cancer and Leukemia
- Inherited Effects
- Embryo and Fetus
What We Know
- Radiation is a weak carcinogen
- The probability of getting cancer is a function of the dose
- No evidence of any cancer effects below about 10 rem
What We Dont Know
- If there are:
- any bad effects below about 10 rem
- beneficial effects below about 10 rem
- any effects other than cancer and leukemia
- any inherited effects at any dose
Important Points
- High normal incidence of cancer (about 30%)
- Cant prove relationship on an individual basis - only an increased relative risk on a large group basis
- Long latent period
- Leukemia - 2 to 7 years from exposure
- Cancer - 10 to 40 or 50 years from exposure
- Dose to tissue
- Cancer wont occur in an organ of the body unless that organ has received a dose
Another Important Point
- Some cancers are not associated with low-to-moderate doses
of ionizing radiation
- Hodgkin's Disease
- Non-Hodgkin's Disease
- Chronic Lymphocytic Leukemia
- Cutaneous Malignant Melanoma
- Uterus
- Prostate
Links
http://www.nas.edu/ssb/besrmenu.html
http://www.rerf.or.jp/eigo/experhp/rerfhome.htm
| Welcome | Contact | Getting Started | Site Map | Project | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 |