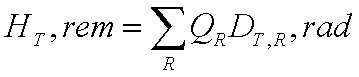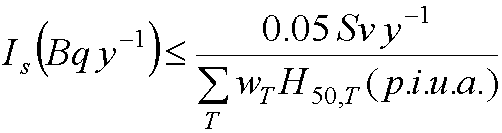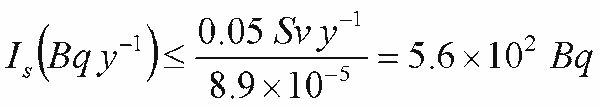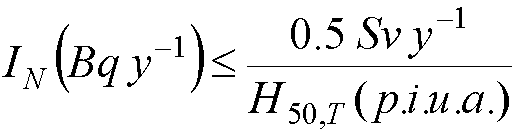Topic 7 - Dose Limits
Our Radiation Dose System |
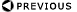 |
 |
- Meandering Through a Complicated Landscape
.
- Cember, Ch 7, 8, 6
Categories of Exposure
- Occupational Exposure
- pregnant workers
- all other radiation workers
- Members of the General Public
- Medical Exposure
Dose Calculation Method(s)
- Dose, at a fundamental level:
- (Energy absorbed)/(mass of material)
- How do you compare doses delivered to different parts of the body?
- Uniform whole body irradiation
- (Most likely) external source
- Gamma emitter
- Non uniform irradiation
- (Most likely) internal source
- a, b, g, N, x-ray or other source
Dose Equivalent (H)
- Biological response varies by radiations
- Radiation weighting factors used to provide a common scale:

- H is the dose equivalent, expressed in Sv
- DT,R is absorbed dose in tissue (T) from radiation (R)
- T is tissue (organ)
- R is radiation type R
- WR is radiation weighting factor
Quality and Radiation Weighting Factors for Various Radiations
| Radiation |
Q
(ICRP20) |
W
(ICRP 60) |
| X, gamma, beta |
1 |
1 |
Neutrons |
|
|
| Thermal |
2 |
5 |
| 0.01 MeV |
2.5 |
10 |
| 0.1 MeV |
7.5 |
10 |
| 0.5 MeV |
11 |
20 |
| > 0.1 - 2 MeV |
|
20 |
| > 2 - 20 MeV |
|
5 |
| Unknown Energy |
10 |
|
| High-energy protons |
10 |
5 |
| Alpha particles, fission fragments, heavy nuclei |
20 |
20 |
Example use of wR
| Radiation |
Measured dose rate µGy h-1 |
WR |
H = D*WR |
| Gammas |
5 |
1 |
5 |
| Thermal neutrons |
2 |
5 |
10 |
| Fast neutrons > 2 MeV |
1 |
5 |
5 |
Does equivalent, H |
20 µSv h-1 |
Traditional Units
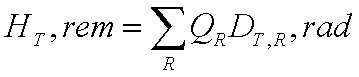
- H is the dose equivalent, expressed in rem
- DT,R is absorbed dose in tissue (T) from radiation (R)
in rads
- T is tissue (organ)
- R is radiation type R
- QR is radiation weighting factor
Internal Dosimetry
- Dose to a person must consider
- Radiation parameters
- Energy
- Half-life
- Radiation type(s)
- Biological parameters
- Organ/body weight
- Biological behavior of contaminant
- Elimination rates
- Calculational techniques
- Metabolic models
- Competing methodologies
- Biological modifiers for radiation types
Accounting for Biological Effects
- Important Note
- The techniques used to calculate biological dose have changed
substantially in the last 30 years
- The terminology used to describe biological dose has not
- The resultant dose predictions have changed, sometimes a lot,
sometimes not at all
- Sorry
- Dose equivalent
- Modifies absorbed dose by a modifying factor
- Accounts for varying biological impacts of different radiations
- Conventional system:
- Rem (Roentgen equivalent man)
- Systeme Internationale:
So
Biological Dose Today
- Measure
- Exposure (X or roentgen) or
- Absorbed dose (rad, Gy)
- Calculate
- Dose equivalent for each effected organ (Gy*WR)
- Result expressed in rem, Sv
History of Internal Dose Calcs
- 1959
- ICRP 2 - Recommendations for Internal and External Exposure
- The recommendations of this organization provided dose limits
from external irradiation (total body) and limited doses to specific
(critical) orgrans. Occupational limits were established:
- total body and gonads, 5 rem/y
- thyroid, skin - 30 rem/y
- skeleton (bone, not marrow) - 0.56 rem/wk (0.1 μCi of
Ra-226)
- all other organs, 15 rem/y
- 1959
- 1960
- 1961
- FRC - Regulations - occupational limits and public exposures
- 1977
- ICRP 26 Recommendations
- New dose limits and the concept of effective dose equivalent
were first introduced.
- 1979
- ICRP 30 - Limits of intakes for workers
- Represents the first complete set of recommendations since the
1950s. Committed dose equivalent, ALI and DACs were introduced for
the first time. Various parts of ICRP 30 were published in the
years following 1979, with updates to dosimetric and metabolic models
being made periodically.
- ~1985
- DOE adopts ICRP 26/30 recommendations (somewhat)
- 1989
- ICRP 56 - Age dependent doses to the public from the intake
of radionuclides
- 1990
- 10 CFR 20 Revision
- NRC publishes the final rule effective 1/1/94.
- Basically adopts ICRP 26 and ICRP 30 with some changes and developments.
- Coins use of TEDE, CEDE, CDE, EDE.
- 1990
- NESHAPS- Limits
- EPA limits radioactive air emissions to 10 mrem dose to public
using ICRP 26/30.
- 1991
- ICRP 60 and 61 - Latest ICRP recommendations, and ALIs/DACs
- New dose limit recommendations based on re-evaluation of risk,
including detriments in addition to fatality.
- New and additional wT values.
- New wR(Q) values.
- Slightly different definitions of terms.
- 1993
- ICRP 67 - Latest ICRP Model
- 1994
- ICRP 66 - Latest ICRP Human Respiratory Tract Model
- 1995
- 10 CFR 834 - (Draft) DOE Dose Limits
ICRP 2 Methodology
- Simple concept
- Still seen in a few regulations
- Assumptions for dose calculations:
- Material defined as soluble
- Can cross body barriers (lung, GI) to move into tissues
- Materials defined as Insoluble (doesnt cross barriers)
- When transmitted to organ(s)
- Uniformly distributed
- Focus on organ with highest concentration or dose
- Focus on occupational exposure
- 40 hrs/wk, 50 wks/yr, 50 yr working life
- Also consider continuous exposure, 168 hrs/wk
- Assume pure parent on intake of nuclide
- Progeny occur after intake
- Compartment model
- Every organ in the body is assumed to be a single compartment
with exponential elimination:

- Employed concept of whole body and critical organ
- Whole body (photon) irradiation can be used to calculate external
dose
- Critical organ
- Calculate dose to a mass of tissue
- Compare doses to all organs
- One with the highest dose is the critical organ
- Dose Rate (D) in organ

- k = proportionality constant (dimensional equalizer)
- q = activity in total body
- f2 = fraction in organ of concern
- e = effective absorbed energy (MeV/dis)
- m = mass of organ
- Buildup to equilibrium from continuous intake also considered:


- Person with continuous intake and constant loss will experience
increase in organ burden over time
Key parameters in ICRP2
- e
- effective absorbed energy
- MeV/dis
- Function of size of tissue
- Values tabulated for various organs
- f2
- fraction in organ of concern
- tabulated for various organs
- tabulated for elements
ICRP 26/30 Philosophy
- Stochastic effects
- were defined as those effects for which the probability
of the effect occuring, rather than its severity, is a function
of dose without a threshold.
- cancer (fatal)
- hereditary (next two generations)
- Non Stochastic Effects
- were those effects for which the severity is a
function of dose and a threshold may exist.
- cataract of lens of the eye (0.15 Sv/y)
- almost any organ in the body can have a nonstochastic effect,
but typically the doses are quite large
- Commited Dose Equivalent
- That dose averaged throughout tissue T over the 50 years after
intake of the radioactive material

- T = tissue T
- t = time
- H = Commited Dose Equivalent
Effective Dose Equivalent (HE)
- Different tissues respond differently to same radiation dose
- Tissue weighting factors used to provide a common scale:

- HE is the effective dose equivalent
- WT is the tissue weighting factor
HE restated
- Effective Dose Equivalent

- HE
- Applies only to stochastic effects
- where wT is the tissue weighting factor
- the fraction of the total stochastic risk associated with
the irradiation of tissue T.
Procedure for Deriving wT
- Identify tissues susceptible to radiation induced cancer
- Establish risk
- Probablity of induction per unit dose equivalent
- Include
- Radiosensitivity
- Essentiallness
- Treatablility
- wT= (risk for tissue T)/(Total Risk)
Deriving Weighting Factors
| Tissue |
Effect |
Risk Coefficient |
ICRP26 Wt |
| Gonads |
Hereditary |
4 * 10-3 Sv-1 |
0.25 |
| Breast |
Cancer |
2.5 * 10-3 Sv-1 |
0.15 |
| Lung |
Cancer |
2 * 10-3 Sv-1 |
0.12 |
| RBM |
Leukemia |
2 * 10-3 Sv-1 |
0.12 |
| Thyroid |
Cancer |
5 * 10-4 Sv-1 |
0.03 |
| Bone Surfaces |
Cancer |
5 * 10-4 Sv-1 |
0.03 |
| Remainder* |
Cancer |
5 * 10-3 Sv-1 |
0.3 (0.06/tissue) |
| Sum Total Risk |
1.65 * 10-2 Sv-1 |
|
| *To use in claculating the effective dose equlivalent,
calculate the dose to the remaining organs, and apply the value of
0.06 to the 5 most-dosed of the remainder, then throw out the rest.
You are then calculating the HE to include up to 11 tissues |
Example
- Laboratory accident results in 185 kBq of 131I uptake
by technician
- 37 kBq to thyroid
- 148 kBq uniformly throughout body
- Doses estimated via scanning/bioassay as:
- 61.5 mSv to thyroid
- 0.13 mSv to whole body
- What was HE?
- HE = 0.05·(61.5) + 0.95 ·(0.13) = 3.2 mSv
ICRP 30 continued
- ICRP 30, the revised 10 CFR 20, and draft DOE 10 CFR 834 are based
on the principle
- that the risk should be equal whether the whole body is irradiated
(external or internal) or whether there is non-uniform, part body
irradiation (external or internal).
- This condition is met if:

- wb = whole body
- wT = tissue weighting factor
- HT = dose equivalent received by tissue T
- Hwb= stochastic dose equivalent limit for uniform
wb irradiation
Limits for Intake by Workers
- Risk estimates of cancer & hereditary effects
- made using the linear dose response relationship.
- Total dose equivalent over the organ/tissue determines the effect,
regardless of the time over which it is delivered.
- For intake limits, 50 years is used as the occupational lifetime.
- Committed Dose Equivalent (CDE) is the total dose equivalent
in any tissue over the 50 years after intake (ref man).

- Committed Effective Dose (Equivalent) (CEDE) is the risk-weighted
sum of committed dose equivalents to tissues (HT,50).

Basic Limits - Occupational Exposure
- The ICRP 26 basic annual limits recommended for exposure to workers
- To limit nonstochastic effects
- 0.5 Sv to all tissues except the lens of the eye
- 0.15 Sv to the lens of the eye
- To limit stochastic effects
- To meet the ICRP 26 basic limits for exposure to workers the intakes
of radioactive material in any year must be limited to satisfy the following
conditions (assuming only internal exposure):

- and

- HT,50 is the committed dose equivalent in tissue, T,
resulting from intakes of radioactive material from all sources during
the year in question.
- The first relationship limits the stochastic effects and the
second limits the non-stochastic effects arising from the intake
of radioactive material.
- Only the annual intake is limited, not the rate of intake.
- Note: 10 CFR 20 defines the Total Effective Dose Equivalent
(TEDE) as the sum of the deep dose equivalent (external dose) and the
committed effective dose equivalent (internal dose). The dose limit
is then based on the TEDE.
Annual Limit on Intake
- Activity of a radionuclide, which if taken in alone, would irradiate
an individual to the limit set by the ICRP for each year of occupational
exposure
- Intake rate: quantity per year
- Pure parent assumption
- Can have an ALI each year
- No time constraint set on exposure period
- (rate can be instantaneous or up to a year)
- Two limits stochastic and nonstochastic considered.
- Secondary limit
- designed to meet the basic limits for occupational exposure
- derived from the previous two relationships.
- The ALI is the greatest value of the annual intake, I, which
satisfies both of the following inequalities:


- Where
- I (Bq) is the annual intake of the specified radionuclide (by
ingestion or inhalation).
- S = stochastic limit
- N = nonstochastic limit
- HT,50 per unit intake (Sv Bq-1) is the
committed dose equivalent in tissue (T) from the intake of unit
activity of the nuclide by the specified route.
- If Is not exceeded, then stochastic limits met
- If In not exceeded, then nonstochastic limits met
- Select value of I which satisfies both inequalities to determine
limiting value.
Calculating an ALI inhalation- example 239 Pu intake by inhalation
| Tissue |
H50,T Sv Bq-1 |
WT |
H50,T Sv * WT |
| Lungs |
3.2 * 10-4 |
0.12 |
309 * 10-5 |
| Red Marrow |
7.6 * 10-5 |
0.12 |
9.1 * 10-6 |
| Bone surfaces |
9.5 * 10-4 |
0.03 |
2.9 * 10-5 |
| Liver |
2.1 * 10-4 |
0.06 |
1.2 * 10-4 |
| Sum |
8.9 * 10-5 Sv Bq-1 |
ICRP 30
Calculating ALI (stochastic)
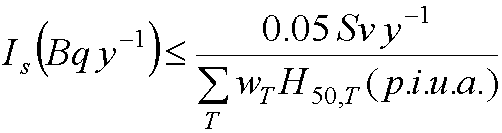
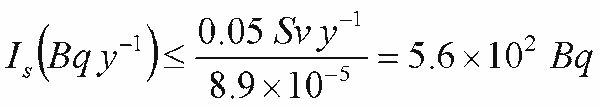
Calculating ALI (nonstochastic)
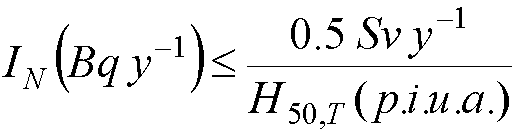
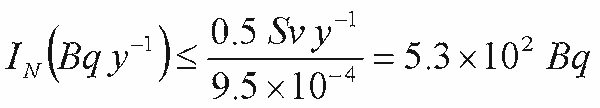
Calculating ALI: 239Pu
- Stochastic limit
- Nonstochastic limit
- Uncertainites in metabolic models result in listed ALI at one significant
figure:
Derived Air Concentrations
- Revised version of ICRP 2 MPCair
- Maximum permissible concentration (air)
- Old MPCs were misused.
- They were maximum permissible concentrations intended
to control exposure over prolonged periods (> 3 mos).
- They have been used to infer over-exposure for even short exposure
times.
- The limit for inhalation of a radionuclide is the appropriate
ALI.
- The concentration of a radionuclide in air during any year is
limited as follows:
- That concentration of a radionuclide in air, which if breathed for
one working year, would result in one ALI by inhalation:

- 2000 hrs per working year
- 1.2 m3 h-1 working breathing rate
- Note: ALI is the main limit and the DAC is a derived limit.
|